Vector Laboratories is closed for the President’s Day on Monday, February 19th. We will be back in the office on Tuesday, February 20th.
We will respond to emails upon our return. Have a wonderful day.
Menu
Vector Laboratories is closed for the President’s Day on Monday, February 19th. We will be back in the office on Tuesday, February 20th.
We will respond to emails upon our return. Have a wonderful day.

Programmed cell death ligand (PD-L1) is one of the major brakes in the body’s immune response to cancer. Binding to the PD-1 protein on T cells, PD-L1 hinders antitumor activity. That’s why PD-L1 upregulation has been associated with poor immune function and increased evasiveness in various cancer types [1].
Despite a number of FDA-approved PD-L1 inhibitors, achieving long-term effects in anti-PD-1/PD-L1 therapy remains a challenge due to certain complexities. The resistance mainly occurs in cold tumors, which have little to no tumor-infiltrating T lymphocytes.
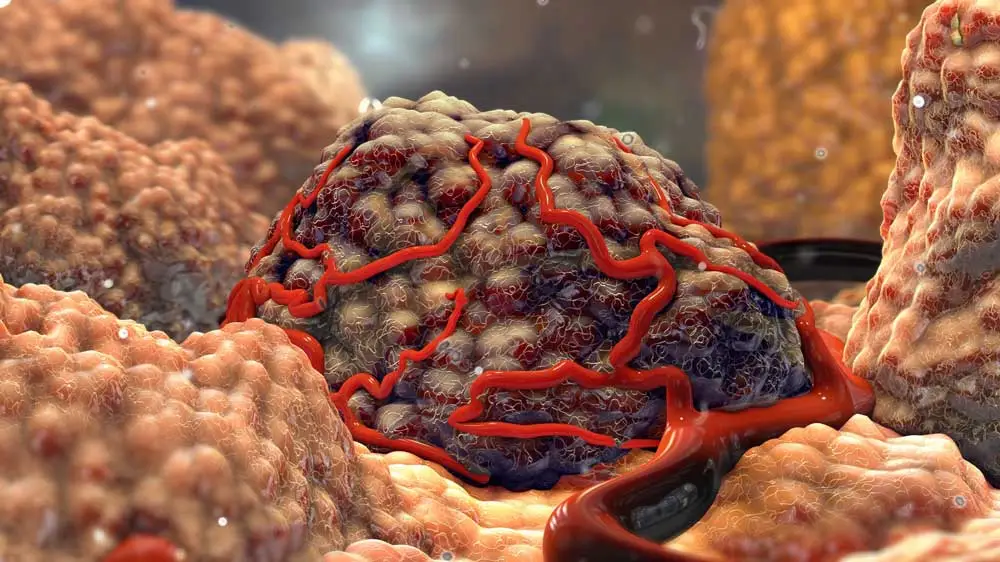
The tumor microenvironment structure makes the infiltration all the more challenging, boasting not only a compact extracellular matrix to prevent accumulation of the PD-L1 inhibitor but also immunosuppressor cells that inhibit T-cell immune response.
The enhanced efficacy of PD-L1 inhibitors requires a multifaceted approach that not only shifts the tumor microenvironment in favor of T-cell function but also alters the tumor structure to allow deeper penetration and accumulation of the inhibitor.
To improve the outcome of PD-L1 inhibitors, researchers at Huazhong University of Science and Technology, China, targeted tumor-associated macrophages (TAMs) [2]. These white blood cells occur in two counteractive phenotypes. While M1-like TAMs induce cytotoxicity by activating T cells, M2-like TAMs inhibit the cytotoxic response by secreting cytokines and immunosuppressive cells. In other words, the overabundance of M2-like TAMs, compared to the M1 type, means that the tumor microenvironment will inhibit T-cell function. By targeting M2-like TAMs, the researchers aimed to repolarize them into M1 phenotype so that the tumor microenvironment would allow PD-L1 inhibitors to fully exhibit anticancer activity.
The study used Metformin (Met), a prescription drug for type-2 diabetes, as the repolarization agent. There is a growing body of evidence documenting Met’s antitumor activities, including its repolarization ability [3]. The only problem was targeted delivery of Met to M2-like TAMs.
To achieve targeted delivery of Met, the researchers used cellular microparticles (MPs). Microparticles have previously been cited in many studies as reliable delivery mechanisms for genetic materials and therapeutics, keeping healthy cells safe thanks to their biocompatibility and low toxicity [4][5][6].
The targeting ability of macrophage-derived microparticles was acquired by engineering them to produce mannose, making them recognizable to the mannose receptor CD206/MRC1, which is highly expressed on M2-like TAM surfaces. Once uptaken by the macrophages, the microparticles could then release Met in a pH-responsive manner.
Leveraging fluorescein-conjugated tomato lectin, followed by intravenous injection of Cy5-conjugated anti-PD-1 antibody, the team was able to label tumor vessels to study the vasculature. This labeling revealed that the anti-PD-1 antibody resulted in extravasation from tumor vessels and enhanced tumor penetration after microparticle treatment.
The research assessed the efficacy of mannose-modified microparticles loaded with Met (Met@Man-MPs) from several angles, examining everything from impact on tumor microenvironment to synergistic effect on anti-PD-1 antibody activity.
Targeting M2-Like TAMs
In vitro studies and in vivo studies confirmed that the mannose modification improved the specific affinity of the microparticles to M2-like TAMs amongst a number of immune cells. Compared to Met in free-form and loaded onto unmodified microparticles, Met carried by mannose-modified microparticles saw the highest level of cellular uptake and intracellular release. The researchers also confirmed that the uptake mechanism involved mannose receptors on M2-like TAM surfaces.
Repolarizing M2-Like TAMs into M1 Phenotype
The study looked at the changes in macrophage marker expression levels to assess repolarization. Upon treatment with Met, the M2-like TAMs saw a decline in the expression of M2 markers and an increase in M1-related markers, indicating a clear shift into an M1-like phenotype. It is important to note that the shift was greatest with the targeted administration of Met with mannose-modified microparticles, compared to free Met and Met loaded onto unmodified microparticles.
The repolarization of M2-like TAMs was confirmed in cell viability tests, where the repolarized TAMs exhibited cytotoxicity toward cancer cell lines. The cytotoxicity stemmed from increased TNF-a expression, an M1-type biomarker. In other words, besides the anticipated effect on anti-PD-L1 therapy, the repolarized macrophages had direct antitumor effects as well.
Changes in Tumor Microenvironment
The in vivo activity of the targeted macrophages was evaluated in H22 tumor-bearing mice. Intravenous injection of Met-bearing microparticles significantly reduced tumor volume. As expected, the mannose treatment of microparticles increased the bioavailability of Met to the tumor microenvironment.
Looking at the tumor microenvironment content, the researchers found that the targeted macrophages increased activation of several T-cell types while decreasing the number of regulatory cells and myeloid-derived suppressor cells, which would otherwise inhibit T-cell function.
Tumor Collagen Degradation
Since one of the main challenges of anti-PD-L1 therapy was the lack of T-cell infiltration into tumor interiors, the degradation of tumor collagen was a significant milestone. Because the mannose-modified microparticles were macrophage-derived, they expressed the same matrix metalloproteinase (MMP) as the parent macrophages. More importantly, neither mannose modification nor loading of Met disrupted the degradation activity of MMP in microparticles.
In vivo studies of H22 tumor-bearing mice, coupled with immunofluorescence analysis, revealed that MMP significantly reduced the tumor collagen area. Further analysis showed that the number of CD8+ T cells in the tumor interior increased upon treatment with the mannose-modified microparticles containing Met, confirming the contribution of degradation by MMP to deeper T-cell penetration.
Enhanced Anti-PD-1 Antibody Activity
The final evaluation criteria and perhaps the most important one was to explore the impact of microparticle-based targeted delivery of Met on the actual success of anti-PD-1 antibodies.
The researchers constructed a dorsal skin window chamber model to monitor the penetration of anti-PD-1 antibodies across tumor vasculature. Upon treatment with either PBS or Met-loaded microparticles, the tumor vessels were labeled by fluorescein-conjugated tomato lectin (green), followed by intravenous injection with Cy5-conjugated anti-PD-1 antibody (red). Real-time imaging via confocal microscopy, where fluorescein and Cy5 were excited with different lasers, was used to display the extravasation of the anti-PD-1 antibody.
In the control group treated with PBS, the antibody could only congregate around the tumor vessels, whereas the treatment with microparticles enabled a wider antibody distribution throughout the tumor tissue.
While both anti-PD-1 antibody and microparticles with Met exhibited anticancer activity on their own, their combined administration created a synergistic effect that enhanced the overall anticancer effect. At the end of the treatment, 60% of the mice were completely tumor-free. The researchers also noted a 100% survival rate, higher than their previous study groups, which confirmed the biosafety of the microparticles.
One final test was to find out how the immune system of the mice would react in cases of tumor recurrence. Because the combined administration of microparticles and the antibody also increased the CD8+ effector memory T-cell activity, the mice in the treatment group completely rejected the readministered tumor, while the control group saw a re-emergence of tumor growth.
Despite the promising results presented above, the translation of this study into a clinical setting could face a few hurdles. For instance, the mice were treated with microparticles derived from immortalized cells, but such macrophages could prompt an immune attack from the human body. An alternative would be to use human macrophage-derived microparticles, but this would require finding suitable donors.
Nevertheless, the targeted delivery of Met via macrophage-derived microparticles poses great potential, shifting tumor lymphocytes to a phenotype that favors T-cell activity as well as improved tumor infiltration and antibody activity.
References
[1] Patel, Sandip Pravin, and Razelle Kurzrock. 2015. PD-L1 expression as a predictive biomarker in cancer immunotherapy. Molecular Cancer Therapeutics 14.4 (2015): 847-856.
[2] Wei, Zhaohan et al. 2021. Boosting anti-PD-1 therapy with metformin-loaded macrophage-derived microparticles. Nature Communications. 12 (2021): 440.
[3] Chiang, Chi-Fu, et al. 2017. Metformin-treated cancer cells modulate macrophage polarization through AMPK-NF-κB signaling. Oncotarget 8.13 (2017): 20706.
[4] Kao, Chen-Yuan, and Eleftherios T. Papoutsakis. 2018. Engineering human megakaryocytic microparticles for targeted delivery of nucleic acids to hematopoietic stem and progenitor cells. Science Advances 4.11 (2018): eaau6762.
[5] Chen, Gang, et al. Transformation of cell‐derived microparticles into quantum‐dot‐labeled nanovectors for antitumor siRNA delivery. Angewandte Chemie 127.3 (2015): 1050-1054.
[6] Tang, Ke, et al. 2012. Delivery of chemotherapeutic drugs in tumour cell-derived microparticles. Nature Communications 3.1 (2012): 1-11.




Stay in the Loop. Join Our Online Community
Together we breakthroughTM

©Vector Laboratories, Inc. 2024 All Rights Reserved.