Vector Laboratories is closed for the President’s Day on Monday, February 19th. We will be back in the office on Tuesday, February 20th.
We will respond to emails upon our return. Have a wonderful day.
Menu
Vector Laboratories is closed for the President’s Day on Monday, February 19th. We will be back in the office on Tuesday, February 20th.
We will respond to emails upon our return. Have a wonderful day.


Scientists facing a research problem often look for innovative ways to challenge the status quo to drive change. For Shuying (Linda) Xu, a third-year PhD candidate at Tufts University, Boston Massachusetts, that involves a focus on neutrophil cell therapy as an option for treating pneumonia, which can have severe complications after an active infection.
“One of the things that my boss always likes to say is that medicine now is like a Bandaid—people have a problem, you put a Bandaid on it, and hopefully it goes away. But the idea of cell therapy is to harness the powers our innate ability to deal with some of these things or boost our system so that we can get closer to an actual cure.”
While the possibility of using immune cell therapy based on the components in blood has been under study since blood transfusions became possible, it has been technically difficult to pursue. Since neutrophils are a short-lived cell with a lifetime of about a day, the logistics of cell therapy with them would require donations and transfusions to occur on the same day. That is, unless you figure out how to engineer neutrophils to have a longer lifespan. For now, this breakthrough discovery involves cell therapy that relies on neutrophil progenitor cells for the transfusion that ultimately will differentiate into neutrophils inside the body. This is still only half the battle, as controlling the superpowers of the neutrophil to make it more suitable as a cell therapy option requires technology that can enhance for its good characteristics and suppress the more detrimental ones. Linda believes that neutrophils may lead to the potentially fatal systemic complications after the infection escapes from the lungs and enters the blood stream to cause sepsis. She hopes that neutrophil cell therapy can provide a means to limit pneumonia to a local infection of the lungs and reduce the possibility of it escalating to a systemic infection.
“I focus on the neutrophil aspects of pneumonia, looking at how it is a double-edged sword that both helps and can be detrimental to infection. Neutrophils make of the bulk of white blood cells in your body and act like the first responders to the scene of any infection. But when you have pneumonia, the neutrophils turn into a super-inflammatory cell type carrying an arsenal of weapons, which can cause a lot more inflammation and tissue damage than you want.”
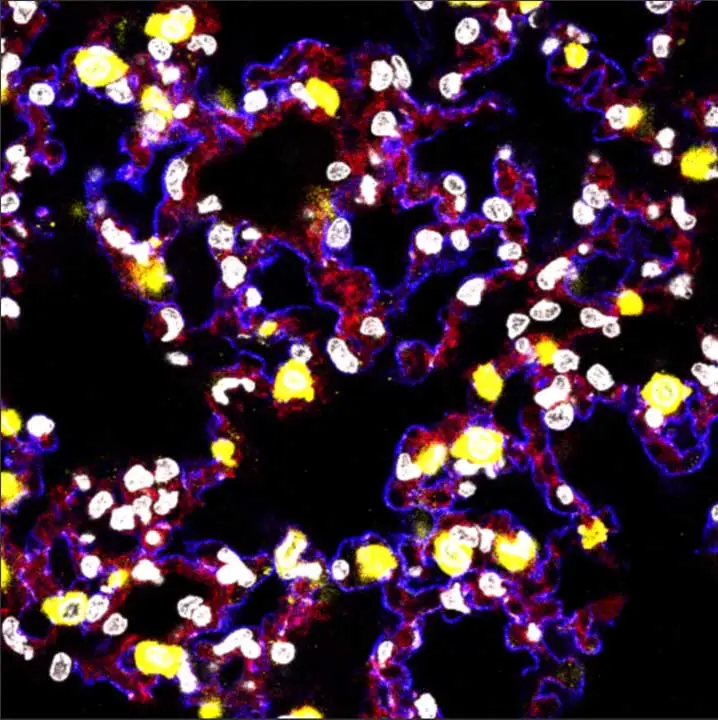
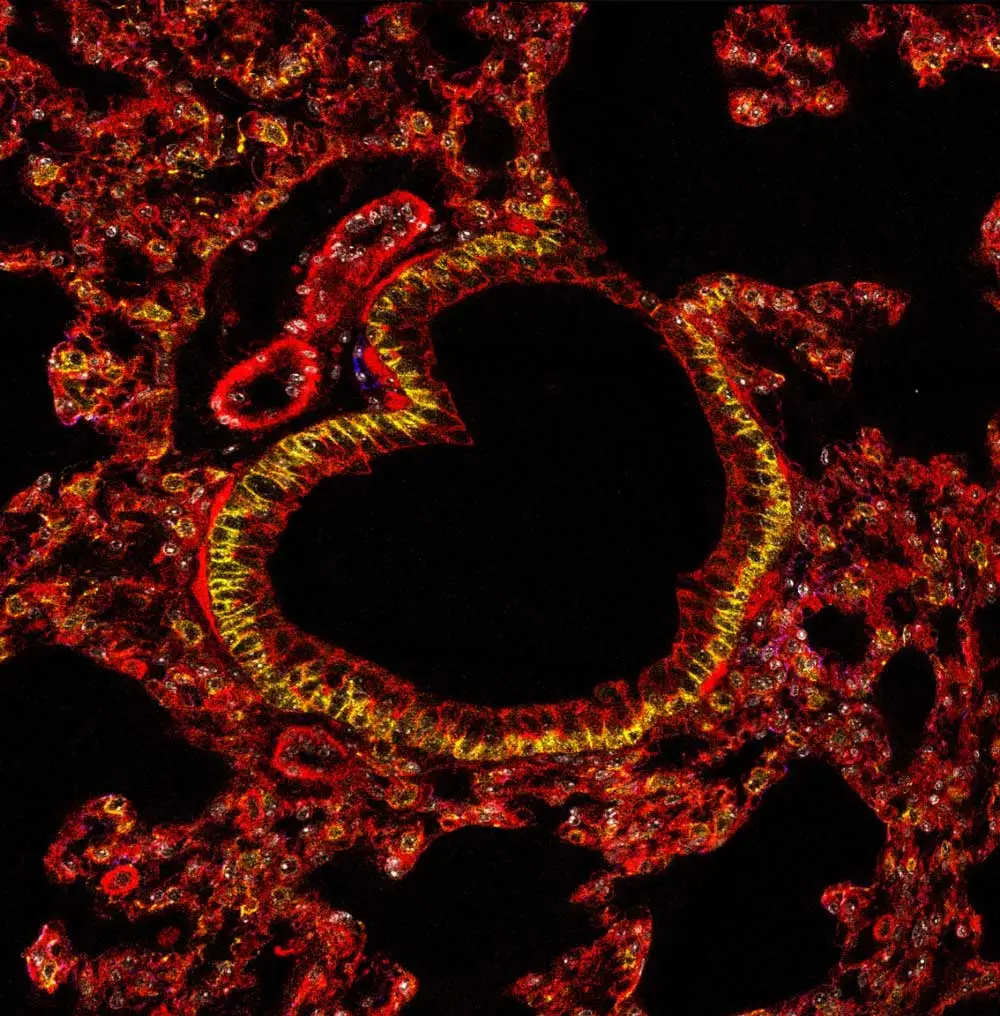
Studying Streptococcal pneumonia and infection is complicated by the challenges of studying the lungs: where in vitro systems are lacking to understand its barrier functions, cell lines may not have the right junctions, and the autofluorescence of lung tissues can interfere with microscopy. Despite these hurdles, Linda has been able to make some adjustments so that the patient stem cells she now uses for modeling that do represent the barrier functions and can maintain an air-liquid interface. Her in vivo imaging technique integrates VECTASHIELD Antifade Mounting Medium to help maintain fluorescence in her samples long enough to enable a second look. Linda feels that being able to visualize biological processes right before one’s eyes can indeed provide a great deal of insight, ensuring that imagery captures not only the beauty but also persists long enough to capture and interpret the role of the neutrophil in the process is vital.
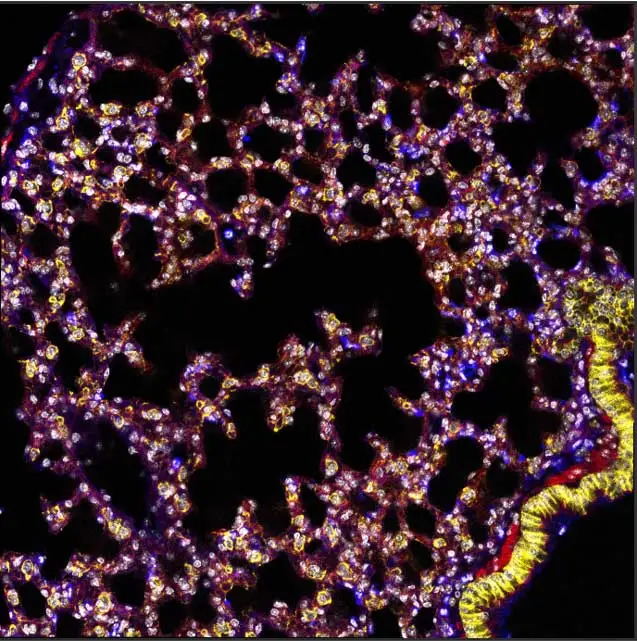
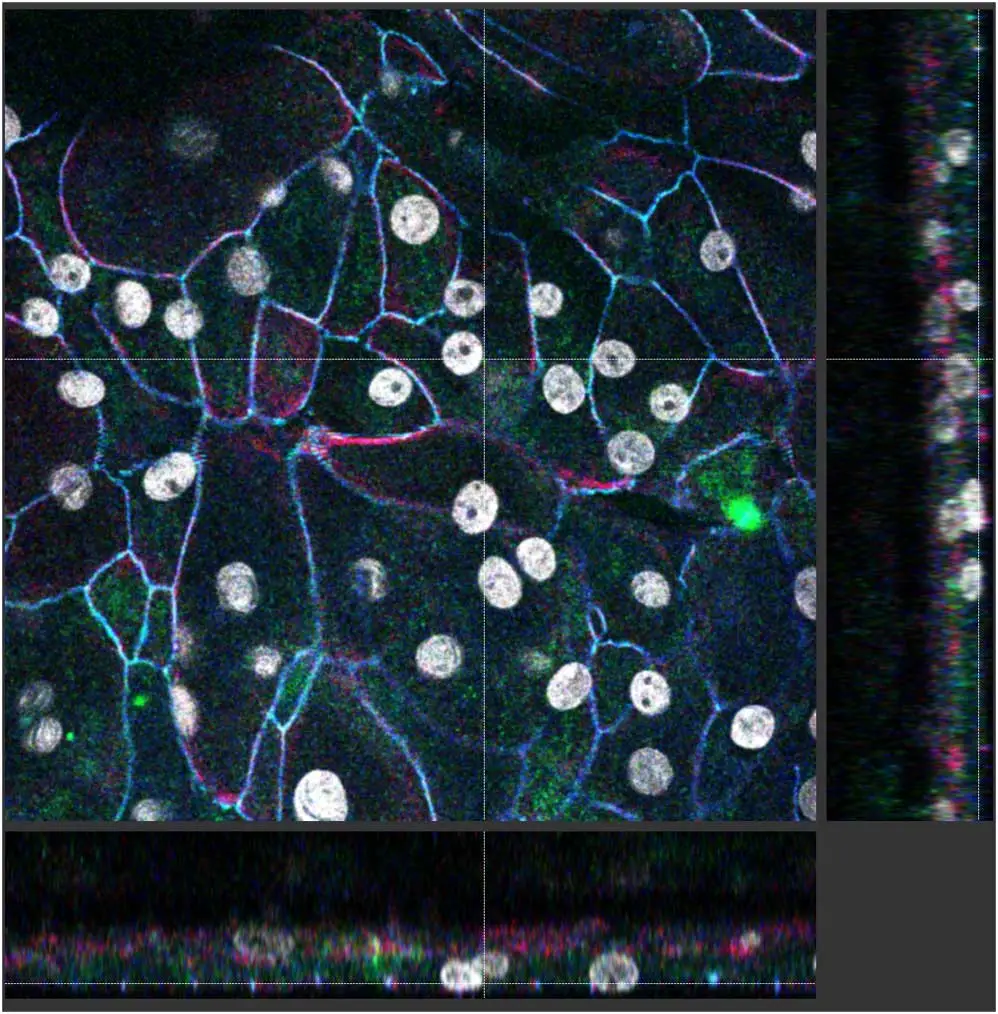
Linda is leaning toward pursuing a career in academia as part of her current five-year plan to align with her research or teaching interests, or both. However, her curiosity also is piqued by the unlimited opportunities available in Boston, a thriving startup and biotechnology hub. Nevertheless, she is unwavering in her attraction to science, which she traces back to her teenage years in Vancouver, Canada. She describes this as the “nerdy aspects of me that likes things like phylogeny and all the different forms of life” and fondly recalls the awe she felt dissecting planaria in science lab and seeing first-hand their extraordinary regeneration ability. This early interest matured into a great appreciation for the more practical and rewarding aspects where science can provide benefits in healthcare and treatment options. Alongside her technical interests, Linda brings a love of art and teaching into her work. She enjoys painting, drawing, and digital art. When she teaches summer students science and immunology, she integrates visual aids and animations of her own design to better explain the concepts.
After moving to the Boston area after earning her BA in Biochemistry from Mount Holyoke College (South Hadley, Massachusetts), she found satisfaction as a Research Technician in the Division of Infectious Diseases at Massachusetts General Hospital and developed her interest in neutrophils, which she now believes are “the coolest white blood cell”. She chose her graduate school based on this and wanted to have a microscopy-heavy project. To Linda, seeing is believing–and compelling in terms of the science—but it also feels good to look at an image that also looks great, even if it isn’t as quantitative as disciplines with lots of numeric data.
“Tufts is a smaller graduate school. But because of its smaller size, it’s more graduate-student focused… PIs have to rely on us graduate students to produce their work and, because they focus on training us, we end up getting more of their attention, as well. For example, our Immunology department may gain three PhD students a year. When I learned about the lab here that studies neutrophils and uses pneumonia as a model, I thought Tufts would be a good fit for me.”




Stay in the Loop. Join Our Online Community
Together we breakthroughTM

©Vector Laboratories, Inc. 2024 All Rights Reserved.